
Developing effective health leaders: the critical elements for success
Introduction
When things go ‘wrong’ in our hospital system, quality health leadership is often recognised by its absence as much as by its presence. Exhaustive research by Health Workforce Australia (HWA) in 2012 concluded that a large body of evidence exists maintaining that the quality of leadership affects people’s satisfaction, trust in management, commitment, individual and team effectiveness, the culture and climate of organisations, and ultimately individual and collective performance. Health is recognised for its complexity and the quality of health leadership directly and indirectly affects the quality of patient care (1). Importantly, leadership plays a central role in mobilising people towards a common goal (2).
The need for ‘leadership development’ in healthcare is being seen as a strategic imperative by both health services, and by professional associations whose role it is to support leader development, defined at an individual level as the “expansion of a person’s capacity to be effective in leadership roles and processes” (3). What enhances that effectiveness through the process of leadership development, is self-management capabilities, social capabilities and work facilitation capabilities (skills in management, strategic thinking, change management) (3). The focus of this article will be on leader development as one aspect of leadership development in the context of the healthcare environment and, the role that a professional association like the ACHSM, can play in offering critical leadership development processes.
The ACHSM was cooperatively established in Australia to facilitate and recognise leadership development in healthcare. Since its inception in 1945, originally called the Australian Institute of Hospital Administrators, ACHSM National Congresses have been used to bring together health leaders from around the country to share new thinking, reflect on international and local developments in health policy and management, as well as grow professional networks. Those networks have frequently evolved to research collaboratives, study tours, and career enhancing opportunities.
Formal development of health leaders has always been an important foundation for understanding the complexities of the business of healthcare delivery. The first Institute of Hospital Administration course was established in 1947 which served as the genesis of the establishment of the School of Hospital Administration at the University of New South Wales where many post 1968 health leader gained their formal graduate qualifications and went on to manage multi-million-dollar healthcare organisations. It represented the formalisation of learning for aspiring health leaders.
In 1996 formal relationships were established with both New Zealand and Hong Kong to expand healthcare networks into the Asia-Pacific Region. But it was not until 2018 that an ACHSM Branch was established in India recognising the expanded role of Australian Universities servicing both Indian and Chinese students in medicine and healthcare. This raised awareness within ACHSM of the cultural context of leadership development particularly in relation to critical thinking.
Partnerships were recognised as critical element in leadership development. In 1996 ACHSM established a formal relationship with the Society of Health Administration Programs in Education (SHAPE). This was designed to promote research and bring further academic rigour and collaboration in the teaching of health administration.
In 2000, a formal and certificated Continuing Professional Development Program (CPD) was introduced as a requirement for all ACHSM members active in health services management. ACHSM Branches were all required to have an active professional development event calendar to provide a forum for exploring new policy initiatives and leading-edge management approaches to addressing challenges in health service organisation and delivery.
Discussion
There is an assumption in this article that leaders can be developed. In considering appropriate strategies for the development of effective health leaders, it is perhaps important to appreciate that what constitute a highly functioning health service leader, possessing the required strategic skills, articulating a clear vision and direction for their organisation, is influenced by a rich and diverse context.
The context of a health manager is a health system which is inherently complex, dominated by a significant number of highly influential professional groups, often politically impacted at a policy level, and experiencing constant cycles of change (4). That change is particularly noticeable in the rapid advances in medical technology, drug therapies, and health information systems, all placing cost pressures on the health system and health leaders managing limited resources.
The more recent management focus on patient safety, continuous quality improvement and the need to demonstrate a positive organisational culture, has compounded the already significant challenge for health leaders of balancing budgets and meeting performance targets. These recent expectations are all set against a backdrop of heightened expectation of greater management accountability and transparency for performance, established by both governments and health Boards. A good example is the ‘Victorian health services Performance Monitoring Framework’ (5). Any leadership development strategy needs to address this complexity and competing demands when deciding required management competencies. McDermott et al. maintain that the industry in which an organisation is embedded, influences the adoption of certain types of leadership approaches with healthcare organisations tending to adopt collective or social leadership strategies (6). In the health sector, effective leaders are required to manage ‘inter-group relationships’ and to manage the medical-management interface (6).
A further consideration when it comes to leadership development is the role that health managers play. The design of health organisations inevitably incorporate duality in the role of more experienced clinicians. These clinicians, whether medical, nursing, or allied health, will inevitably be asked to step up to managerial positions in a health organisation. McKenna and Richardson maintain that the literature poorly reflects the ‘complexity and difficulty of the managerial experience (7). This difficulty is compounded when highly qualified and skilled clinician managers, who do not possess any formal management qualifications or training, assume managerial roles. Fitzgerald and Teal highlight the significant tension between clinical identity, the work, and the management role, which is also influential in increasing the complexity of the management task and commensurate capabilities required to manage those tasks effectively (8).
Not-with-standing clinician/managers lacking formal management education, they do possess deep contextual understanding of the health management problems, and exercise the role of ‘sensemaking’ which gives them significant credibility in persuading clinical colleagues when it comes to encouraging change (9). The understanding of professional sub-cultures in healthcare is also critical to the enactment of management roles, and learning the skill of negotiation through formal and informal accountabilities (10). This understanding is critical to leadership development in healthcare, as it is a primary determinant of successful change management to clinical processes in hospitals.
It is important to recognise that leadership education is different from leadership development. Leadership education relates to the content about leadership and leadership theories, and leadership development concentrates on the process through which leadership knowledge, skills, and abilities are created (11). When addressing what constitutes the ‘content’ of leadership, leadership competency and capability frameworks assist the articulation of the industry expectation of the role, knowledge and behaviours of a health leader. How do employers, be they governments or Boards of Directors, select, train, and performance manage or review, their health leaders? What are the critical elements to guide the educational institutions as to what is important in health management education?
The public sector utilises leadership frameworks for leadership development in Queensland (12), New South Wales (13), South Australia (14), Western Australia (15), and Victoria (16). Internationally, leadership frameworks from USA, the United Kingdom NHS Leadership Framework 2011 (17) later to become the NHS Leadership Model 2016, and in particular the Canadian Health LEADS (18), influenced the development of the Australia Health Leadership Framework 2013 (19). These leadership frameworks have normally had a human resources function of guiding the selection and development of managers on the pathway to a leadership career, but they are also a useful guide to the evolving content of leadership used in education and research. Hartley’s review of the healthcare leadership literature concluded that a key leadership skill was ‘reading the context’ in healthcare and that is when leaders become effective in the domain of ‘leadership and change management’ (20). Health leaders also need to improve their skills and become competent in relationship management, required when negotiating process change with highly skilled health professional groups.
A key question is whether there is a real difference between leadership capability and leadership competence when it comes to the development of leadership frameworks? It would appear from the literature that a person with a capability has a potential to acquire a specific ability or skill that will make them more capable to complete a certain task or make them a more suitable candidate for a job. With practice, capabilities can develop into competence. Therefore, leadership competency of a health leader constitutes the possession of particular leadership skills, knowledge, attitudes, and capacities to fulfil their organisation’s needs and demonstrate behaviours that contribute to superior organisational performance. By using a competency-based approach to leadership, organisations have been in a better position to identify and develop their next generation of health leaders. Similarly, Universities and professional associations, like the ACHSM, have been able to use agreed management and leadership competency frameworks, to frame appropriate academic curriculum and professional development activities and processes, based on the specified content and competencies articulated in those management competency frameworks.
Leadership capability focuses more on the ability to develop to meet future organisational needs. It is associated with the ability to lead, inspire, direct, and teach others in the organisation. Fraser and Greenhalgh (21) define capability as the “extent to which individuals can adapt to change, generate new knowledge, and continue to improve their performance”. They argue capability is important in meeting constantly changing needs and continuously evolving organisations. Traditional approaches to management education and training tend to focus on enhancing competence, whereas Fraser and Greenhalgh maintain that in the complex contexts associated with healthcare, it is important to educate for capability. Educating for capability would include performance feedback, being challenged by unfamiliar contexts, and identification of personalised learning goals, feedback, reflection and consolidation (21).
Briggs et al. correctly identified this management learning should go further beyond experiential and contextual learning, to include, amongst others, personal traits that emphasise integrity, the generation of organisational trust, and the building of resilience (4). McCauley and Van Velsor importantly add values like engendering credibility in others, personal initiative and drive, and optimistic attitude (3). These traits are highly important in facilitating meaningful organisational change, demonstrating professional responsibility, and ensuring personal survival in the challenging and complex world of health service management.
Turning to the process of leadership development, an important consideration is the role of emotion in leader development. Given the work of Goleman (22) who maintained that the leader’s ability to understand, manage, and use emotional awareness (a leader’s emotional intelligence), enhances the quality of relationships and improves reactions to problematic individuals and situations, consideration needs to be given to emotions in suitable leadership development processes. According to McDermott et al., when healthcare leaders adopt collective leadership strategies, then leaders’ engagement in self-reflection enables a broader development which contributes to a stronger sense of self-identity and understanding of those around them, as occurs through mentoring (6). As leadership is an inherently social role where leaders need to complete organisational tasks through their people, emotional skills are a critical part of a leader’s development and ultimately their effectiveness.
There is a significant volume of literature surrounding what constitutes effective approaches to leadership development. Gonin et al. concluded that traditional classroom based educational approaches to leadership development were less effective than (I) coaching and mentoring, (II) leaders teaching leaders, (III) action learning, (IV) peer networking and learning, as well as (V) external insights from customers/suppliers (23).
Mumford’s research found that increased levels of leadership skills relating to such things as knowledge, problem-solving skills, and system skills, found at higher positions of leadership. Certain other skills were more relevant at other organisational levels leading to the conclusion that leadership development in its very nature is progressive and systematic. Furthermore, leader development involves an interplay of personal characteristics, early experiences and career-related learnings (24).
Boak and Crabbe discovered that with mature managers, facing work challenges, contributing to major decisions, and taking on new responsibilities, rated highly as part of their leadership development. This was particularly true of experiences in the last 5 years. Other experiences judged to have a positive impact on development were learning from others and acting as a mentor to others (25).
Action learning projects and ‘Leadership Learning Sets’ are a commonly used leadership development process for more senior health leaders. Raelin et al. (26) had espoused the value of collaborative working and learning in leadership development. Challenging experiences and the response to “what keeps you awake at night?” question in a learning set, requires managers to try new behaviours and to reframe old ways of thinking and acting. Miller et al. (27) outline the methodology of five phases of the Learning Sets used by National Public Health Leadership Institute (PHLI) and the five learning methods that they utilised. Their research showed that ‘declarative knowledge’, or having the knowledge of something, is not sufficient to achieve leadership learning outcomes. The development of ‘procedural knowledge’, or knowledge of how to do something, should be the focus. Procedural knowledge is in itself dynamic, so that this knowledge changes in its application and meaning according to the context.
Action learning is focused on developing such procedural knowledge through asking participants to address complex situations or problems that they bring to the Learning Set, apply new leadership perspectives and actions to address those problems, and reflect on how it all went and what they would do in the future to achieve greater success. After 13 years of evaluation results with Learning Sets, PHLI’s research concluded using multiple methods increases learning for individual participants in leadership development and improves outcomes for organisations (27).
If leadership development can be viewed as an acquired skill gained over time with the right experiences, what is the best way to train emerging health leaders? Mumford et al. recognised four career-specific methods for leadership development and these included (I) job assignments that provide exposure to challenging problems (II) mentoring (III) appropriate training and (IV) practical experience in solving work related problems (24). Therefore, critical to leadership development is addressing practical workplace challenges, not only refining leadership problem-solving skills of the emerging health leader, but to reinforcing their learning. Leadership development is largely a collective and social process that is most successful when performed addressing the complexities real world healthcare issues and problems (24). Turner et al., like Hartley et al., maintain that leadership development is contextual and that leadership development design (which could include one or more of 500 different leadership development techniques) should accommodate contextual issues with all stakeholders (individual or collective) (11).
As a consequence, considering leader development is contextual, over the 74-year history of ACHSM there were ongoing debates about what were the appropriate management competencies effective healthcare leaders required, in order to be judged proficient. Financial skills featured heavily because financial performance was rated highly by hospital and health service Boards, as well the Departments of Health, around Australia. This was due to hospital budgets always being constrained and challenged by significant wage growth, as well as evolving expensive medical technologies and innovation in pharmaceuticals. This was not dissimilar to the international focus on financial performance by the Harvard Business Review (HBR) who ranked and published the top CEOs each year. However, in 2015 HBR broadened its focus considering environmental, social and governance performance in its criteria for top CEOs, reflecting a shift in community attitudes to a more balanced approach in assessing leadership performance. This reflects a similar trend occurring in healthcare in weighing up a health CEO’s contribution to driving value and health outcomes, quality and safety, as well as a good patient experience.
Broad content knowledge of the healthcare management subject areas is vital to be regarded as a competent health leader. Health management academics have shaped the thinking around much of the content of their academic offerings and it was only in 1990 that the first accreditation of health management academic programs was conducted by ACHSM. There was now a mechanism for ACHSM, as a professional College, to ensure its members who are developing their formal skills, are doing so from an accredited University which had undergone a rigorous health sector peer review of their courses and academic staff, particularly pertaining to industry relevance of their course content.
Significant research was undertaken by Liang et al. at La Trobe University in 2010, initially in partnership with ACHSM, where there had been growing interest, to identify health management competencies that were seen to be relevant to the four levels of hospital management and three levels of community health services. These management competencies were identified through a four-stage mixed methods approach first published by Liang et al. in 2012 and refined over the next 6 years. The six competencies identified included: (I) evidence-informed decision-making; (II) operations, administration, and resource management; (III) knowledge of healthcare environment and the organisation; (IV) inter-personal, communication qualities and relationship management; (V) leading people and organisation and (VI) enabling and managing change (28).
Liang’s research has provided valuable guidance to human resource departments within the health system, providing much needed focus as to the six skill areas to be developed in the training of emerging health leaders.
However, attempts like that undertaken by Liang, to define the role of a health manager, and match the required capabilities, in a complex, professionally dominated and highly politically charged health system, frequently experiencing change, is problematic. Briggs et al. also argued that contextualisation was important, and that while competency was about the acquisition and utilisation of skills, this was insufficient to develop an effective health manager. They argued what was equally important was the capacity of a health leader to adapt, change, respond, and improve performance (4).
As outlined earlier, internationally, numerous healthcare professional associations, needing to enhance the skills of its members, had developed management competency frameworks. Set against the background of the development of the Health LEADS Australia Health Leadership Framework of 2013, and under the auspice of The International Hospital Federation (IHF), there were international discussions occurring to build consensus around a global health leadership framework.
An IHF initiative involving a global consortium of 18 countries and professional associations for healthcare management, had done extensive work between January 2013 and June 2015. The influential organisations in the consortium included the American College of Healthcare Executives, Australasian College of Health Service Management, Canadian College of Health Leaders, European Association of Hospital Managers, Hong Kong College of Healthcare Executives and Taiwan College of Healthcare Managers.
All the participants from these health professional organisations were keen to promote healthcare management professionalisation supported by universally recognised health management competencies that would enhance healthcare leadership development in their respective communities. In addition, more than one hundred healthcare professionals and academics contributed to this open review process. What was achieved was an international consensus as to what would be the foundation of health professional education and development on a global scale.
It was in August 2016 that ACHSM agreed with New Zealand and Hong Kong to adopt a Master Health Service Management Competency Framework (Figure 1). ACHSM recognised that healthcare performance improvement was dependent on the quality of professional management and health leadership of its healthcare organisations.
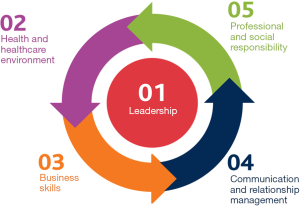
This framework was based on the original work of Stefl (29) who had reached consensus with six major health professional associations who have a coverage of more than 100,000 US health management professionals on what was called The Healthcare Leadership Alliance Competency Model. The significance of Stefl’s research on the HLA Competency Model was the identification of 232 common management competencies organised into five domains then stratified using the Dreyfus framework to distinguish the performance expectations for entry-level, mid-career and senior level health managers. Progression across five skill levels identified by Dreyfus typically required work experience coupled with guided reflection.
The ACHSM Master Health Service Management Competency Framework became the focus of all ACHSM processes including the accreditation of Australasian health management university courses, the ACHSM Fellowship Program, the ACHSM Mentoring Program, all ACHSM continuing professional development activities, and the ACHSM Management Internship Programs.
ACHSM recognised the value of professional mentoring as another critical element of health leader development. It was designed to assist the progression throughout a health manager’s career stages, as well as the value of continued professional development and lifelong learning. While formal University health management education and College professional development activities have been undertaken over many decades, experientially guided learning through mentoring was formally commenced in Victoria in 2001. The ACHSM Mentoring Program was well structured and evidence-based with the requirement of a mutually agreed twelve-month Professional Development Plan with clear development goals and agreed actions. Guidelines for Mentors and Mentees were provided during an orientation session, stressing the importance of building trust relationships, networking, career transitions, and the development of ACHSM management competencies. This 12-month ACHSM Mentoring Program has grown in popularity, and has expanded nationally, not only as a critical one-on-one professional development tool, but in developing lasting relationships between more senior health leader acting as mentors for emerging health leaders.
ACHSM, in close partnership with a major consulting firm, has made Learning Sets available to senior health leaders to facilitate action learning around identified problems in their health organisations. Small groups of health leaders meet four times over a 12-month period in facilitated sharing of ideas and change strategies to real workplace challenges in what might be described as peer-to-peer learning.
The ACHSM Health Management Internship Program followed the Mumford et al. four career-specific methods for leadership development exposing ACHSM management interns to challenging job assignments with hospitals and other health employers facilitated by preceptors (24). In addition, appropriate professional development is provided by ACHSM and a mentor is assigned for the 2 years of the program to assist with the intern’s intrapersonal development. Day had noted that leader development, focussed on intrapersonal competence, should be underpinned by core personal skills that include self-awareness, self-regulation, self-motivation and a shift to relational dialogue (30). Avolio found that effective leaders invest time reflecting on events and use developmental learning from their experiences to guide their future actions (31). Lewis and Jacobs maintained that learning through challenging work roles, and the use of mentoring and coaching as a means of exposing aspiring health leaders to alternative perspectives, were critical leadership development activities (32) and these were all incorporated by ACHSM in their health management internship program.
Finally, ACHSM conducts Fellowship examinations for senior health leaders on an annual basis to reinforce the importance of life-long learning. Candidates join study groups that operate as Learning Sets reviewing and discussing a suite of contemporary health management and policy literature in preparation for the ACHSM Fellowship Viva Examination conducted in Australia and Hong Kong. The focus is demonstrating understanding of the management literature and the application of management theory to practice. The achievement of ACHSM Fellowship is celebrated at the Annual ACHSM Asia-Pacific Congress and represents a significant achievement of gaining the highest status in the College.
Conclusions
The review of research evidence associated with critical elements of leader development has been examined through the lens of a professional association. ACHSM has had a significant role in offering a range of leader development opportunities to senior and emerging health leaders in both Australia and the Asian region, using a wide range of leadership development methodologies.
There appears to be a reasonable evidence base to support the influential role that context, in this case the dynamic and highly complex healthcare environment, plays in both framing the required management competencies and the leader development methodologies, utilised to professionalise health management in Australia. Recent research has focussed on leader development as both an individual and social experience, influenced by specific contextual factors and the career stage of the health leader. It is argued that leader development methodologies should focus on fostering a health leader with ‘context’ understanding, and demonstrated competencies expected by the health industry. In addition, leader development methodologies are more likely to be shown to be effective if they foster procedural knowledge and the capability of the leader to grow and adapt to the challenges of their current health context. Using multiple methods of leader development increases the learning for health leaders if they serve to strengthen their ability to address challenging organisational problems and to think strategically.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editor (Christine Dennis) for the series “Health Service Management” published in Journal of Hospital Management and Health Policy. The article has undergone external peer review.
Conflicts of Interest: The author has completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jhmhp.2019.11.02). The series “Health Service Management” was commissioned by the editorial office without any funding or sponsorship. The author has no other conflicts of interest to declare.
Ethical Statement: The author is accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- HealthWorkforce Australia, Leadership for the sustainability of the health system: Part 1 A literature review. 2012:9. Available online: http://www.springboard.health.nsw.gov.au/content/uploads/2014/07/leadership-for-sustainability-of-health-sector-literature-review-012012.pdf
- Kouzes JM, Posner BZ. The Leadership Challenge. 4th edition. San Francisco CA: Jossey-Bass, 2007:9.
- McCauley CD, Van Velsor E. The Centre for Creative Leadership Development. San Francisco, CA: Jossey-Bass, 2004.
- Briggs DS, Smyth A, Anderson JA. In search of capable health managers: what is distinctive about health management and why does it matter? Asia Pacific Journal of Health Management 2012;7:71-8.
- Department of Health and Human Services. health.vic, Victoria. 2019. Victorian health services Performance Monitoring Framework. Available online: https://www2.health.vic.gov.au/hospitals-and-health-services/funding-performance-accountability/performance-monitoring
- McDermott A, Kidney R, Flood P. Understanding leader development: learning from leaders. Leadership and Organisation Development Journal 2011;32:358-78. [Crossref]
- McKenna S, Richardson J. Managing in the New Zealand health service: the interpretation of experience. J Health Organ Manag 2003;17:74-87. [Crossref] [PubMed]
- Fitzgerald A, Teal G. Health reform, professional identity and occupational sub-cultures: the changing interprofessional relations between doctors and nurses. Contemp Nurse 2003;16:9-19. [PubMed]
- Balogun J, Johnson G. Organisational restructuring and middle manager sensemaking. Acad Manage J 2004;47:523-49.
- Degeling P, Carr A. Leadership for the systematisation of health care: the unaddressed issue in health care reform. J Health Organ Manag 2004;18:399-414. [Crossref] [PubMed]
- Turner JR, Baker R, Schroeder J, et al. Leadership development techniques: Mapping leadership development techniques with leadership capacities using a typology of development. European Journal of Training and Development 2018;42:538-57. [Crossref]
-
Queensland Public Service Capability and Leadership Framework -
NSW Public Sector Capability Framework -
South Australian Executive Service Competency Framework -
Western Australian Commission Leadership Capability Framework - Victorian Health and Human Services Workforce Capability Framework. Available online: http://www.providers.dhhs.vic.gov.au/workforce-capability-tools
-
NHS Leadership Academy Leadership Framework - Canadian College of Health Leaders, LEADS in a Caring Environment (LEADS) framework. Available online: http://www.leadscanada.net/site/framework
- Health Workforce Australia, Health LEADS Australia: The Australian Health Leadership Framework (2013). Available online: http://pandora.nla.gov.au/pan/133228/20150419-0017/www.hwa.gov.au/sites/uploads/Health-LEADS-Australia-A4-FINAL.pdf
- Hartley J, Martin J, Benington J. Leadership in Healthcare: A review of the literature for health care professionals, managers and researchers. Available online: http://www.netscc.ac.uk/hsdr/files/project/SDO_FR_08-1601-148_V01.pdf
- Fraser SW, Greenhalg T. Coping with complexity: educating for capability. BMJ 2001;323:799-803. [Crossref] [PubMed]
- Goleman D. Working with Emotional Intelligence. New York, NY: Bantam Books, 1998.
- Gonin D, Napiersky U, Thorsell J. Innovation in leadership development. Advances in Global Leadership 2011;6:155-215. [Crossref]
- Mumford MD, Marks MA, Connelly MS, et al. Development of leadership skills: experience and timing. Leadersh Q 2000;11:87-114. [Crossref]
- Boak G, Crabbe S. Experiences that develop leadership capabilities. Leadership and Organisation Development Journal 2019;40:97-106. [Crossref]
- Raelin J. Does action learning promote collaborative leadership. Academy of Management Learning and Education 2006;5:152-68. [Crossref]
- Miller DL, Umble KE, Frederick SL, Dinkin DR. Linking learning methods to outcomes in public health leadership development. Leadersh Health Serv (Bradf Engl) 2007;20:97-123. [Crossref] [PubMed]
- Liang Z, Howard PF, Leggat S, et al. Development and validation of health service management competencies. J Health Organ Manag 2018;32:157-75. [Crossref] [PubMed]
- Stefl ME. Common competencies for all healthcare managers: the Healthcare Leadership Alliance model. J Healthc Manag 2008;53:360-73; discussion 374. [Crossref] [PubMed]
- Day DV. Leadership development: a review in context. Leadersh Q 2001;11:581-613. [Crossref]
- Avolio BJ. Leadership Development in Balance: Made/Born. Mahwah, NJ: Lawrence Erlbaum Associates, 2005.
- Lewis PM, Jacobs TO. Individual differences in strategic leadership capacity: a constructive/development view. In: Phillips RL, Hunt JG. editors. Strategic Leadership: A Multi-organisational Perspective, Quorum Books. Westport, CT: Praeger, 1992:121-37.
Cite this article as: Rasa J. Developing effective health leaders: the critical elements for success. J Hosp Manag Health Policy 2020;4:6.

